A Guide to Assisted Conception
Modern reproductive medicine has transformed the landscape for couples and individuals facing fertility challenges. Among the various techniques available, the most prominent and effective is In Vitro Fertilization (IVF). However, the terminology surrounding these procedures—specifically the terms “IVF” and “insemination”—can often be confusing for those beginning their journey. Understanding the IVF Insemination Overview and Definition is the first step toward making informed decisions in fertility care.
Defining the Scope of In Vitro Fertilization
In Vitro Fertilization, or IVF, is a complex series of procedures used to help with fertility or prevent genetic problems and assist with the conception of a child. The Latin term in vitro literally translates to “in glass,” referring to the laboratory environment where fertilization occurs. This process stands in contrast to in vivo fertilization, which takes place naturally within the human body.
While many use the terms “IVF” and “insemination” interchangeably, they refer to different aspects of the reproductive process. In a clinical setting, such as at Liv Hospital, “insemination” typically refers to the specific stage within an IVF cycle where sperm and egg are brought together. It can also refer to Intrauterine Insemination (IUI), a less invasive procedure where sperm is placed directly into the uterus.
The Core Stages of an IVF Cycle
The IVF process is not a single event but a multi-week journey involving several distinct phases. Each phase is critical for the eventual success of the treatment.
1. Ovarian Stimulation and Monitoring
The cycle begins with the administration of injectable hormones to stimulate the ovaries to produce multiple mature eggs, rather than the single egg produced in a natural monthly cycle. This is essential because not all eggs will fertilize or develop into viable embryos. Throughout this 8- to 14-day period, patients undergo regular ultrasounds and blood tests to monitor follicle growth and hormone levels.
2. Egg Retrieval
When the follicles reach the optimal size, a “trigger shot” is administered to finalize egg maturation. Approximately 36 hours later, the eggs are retrieved via a minor surgical procedure. Using ultrasound guidance, a thin needle is passed through the vaginal wall to aspirate the fluid containing the eggs from the follicles. This procedure is typically performed under light sedation to ensure patient comfort.
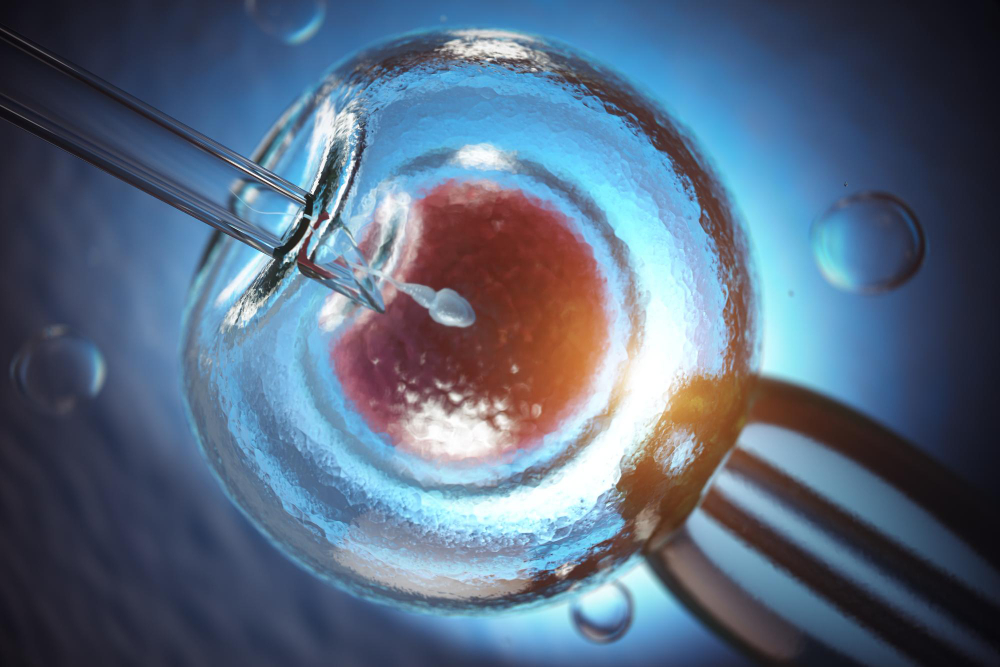
3. The Insemination Phase: Laboratory Fertilization
This is the heart of the IVF process. Once the eggs are retrieved and a sperm sample is collected (or thawed from a donor), they are brought together in a controlled laboratory environment. There are two primary methods for this:
- Conventional Insemination: The eggs are placed in a culture dish with a high concentration of healthy, motile sperm. Fertilization occurs “naturally” in the dish as the sperm swim to and penetrate the egg.
- Intracytoplasmic Sperm Injection (ICSI): If there are concerns regarding sperm count or motility, a single healthy sperm is injected directly into each mature egg using a microscopic needle.
Embryo Development and Transfer
Following insemination, the resulting embryos are cultured in an incubator for three to six days. During this time, embryologists monitor the embryos for proper cell division and growth. In many modern protocols, embryos are allowed to reach the “blastocyst” stage (day 5 or 6), which often has a higher likelihood of successful implantation.
The final clinical step is the embryo transfer. A thin catheter is used to place one or more embryos directly into the uterus. This procedure is generally painless and does not require anesthesia. If the embryo successfully attaches to the uterine lining, pregnancy is achieved.